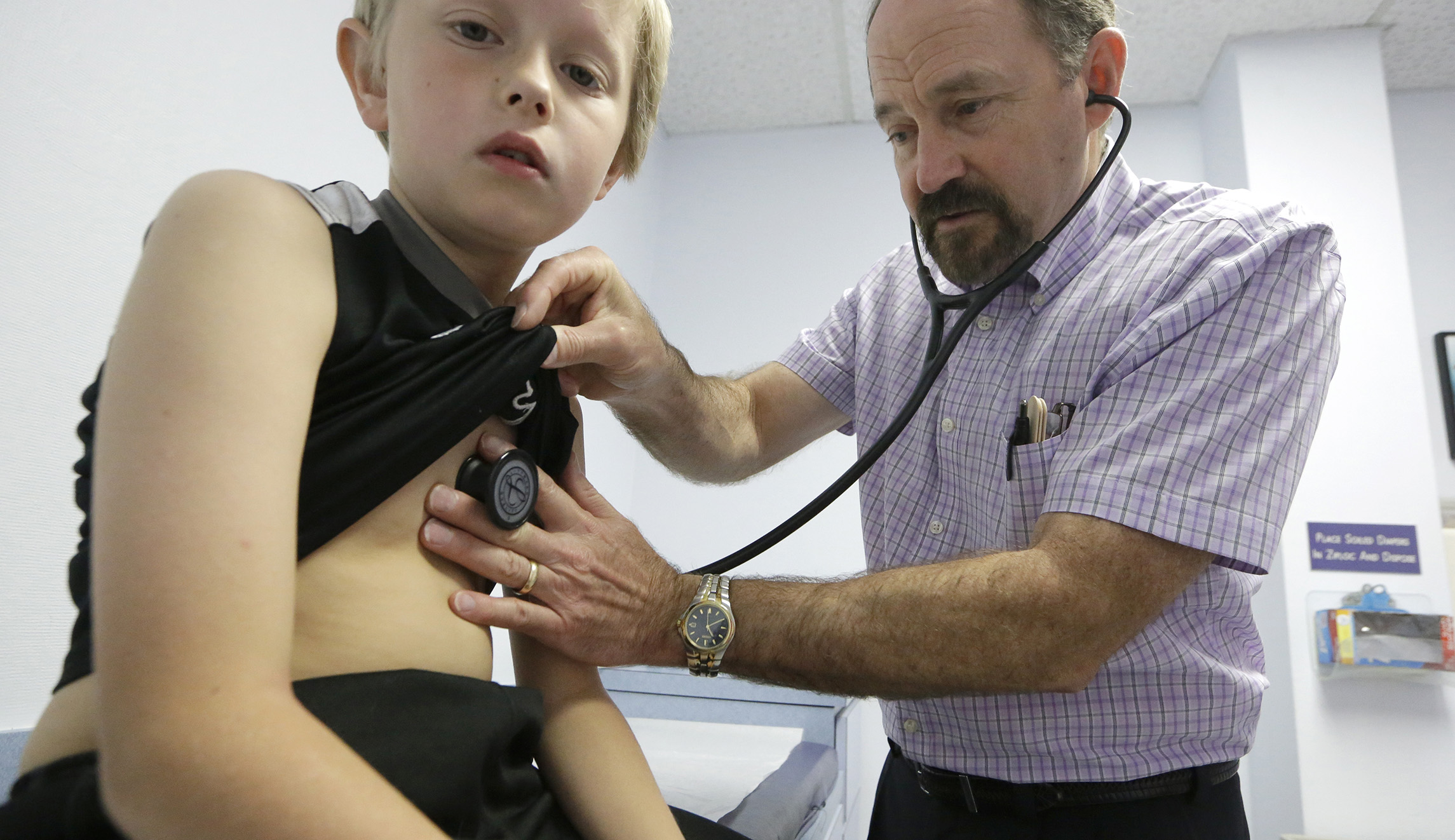
States are facing new problems with the Children’s Health Insurance Program, even as Congress passed a six-year reauthorization for the Children’s Health Insurance Program this week, ending a months-long standoff.
The issues include convincing residents the program still exists and how to grapple with a looming “CHIP cliff.”
Recommended Stories
Advocates and states were relieved that CHIP was funded for six years as part of a short-term deal to fund the federal government until Feb. 8. However, some are concerned about the reason the deal came together: Congressional scorekeepers found that the program will cost less than alternatives for providing care to low-income children, chiefly Medicaid and Obamacare’s subsidized plans.
The Congressional Budget Office found that extending CHIP for a decade would save the federal government $6 billion. That is a drastic change from earlier estimates last year that found the program would cost as much as $8 billion.
A big reason is that alternatives for CHIP such as subsidized Obamacare plans and Medicaid would be more expensive.
But some advocates are worried about what happens with possible changes to Obamacare and Medicaid in the next six years.
“Any actions that Congress and President Trump takes to increase or reduce the costs of either Medicaid or the [Affordable Care Act] during the intervening six years will have an enormous impact on whether we will be able to successfully extend CHIP in 2024 and beyond,” wrote Bruce Lesley, president of the advocacy group Families First, in a post on the website Medium.
Lesley noted that the costs for providing subsidized Obamacare plans are higher than CHIP partly because of the repeal of the law’s individual mandate penalties in tax reform. CBO estimates that premiums could rise 10 percent each year without the fines, which the tax bill repealed started in 2019.
Lesley argues that Congress or the Trump administration could take actions that lower costs for Obamacare or Medicaid and thereby raise costs for CHIP, since that would mean it would cost more to insure someone under CHIP than through Medicaid.
States have to grapple with a CHIP cliff of their own, too.
The six-year extension eliminates a boost to CHIP’s federal matching rate starting in 2020. The average will lower from 93 percent in 2019 to 81.5 percent in 2020 and 70 percent in 2021.
CHIP is a program in which the federal government matches state funding to provide health insurance for children in low-income families. Nearly 9 million children are in the program.
The change to the lower matching rate is to reduce a funding bump that the program received from the Affordable Care Act.
But the phase-in of the cuts happens over several years, giving states time to adjust, said Joan Akler, executive director of the Georgetown University Center for Children and Families, which has tracked changes to the program.
States also have to maintain their current income eligibility levels for CHIP.
Akler is worried, however, that states have a new problem of convincing residents CHIP is still there, especially after the funding lapse that started Sept. 30.
Congress has been mired in partisan fights over how to fund the program. A bill that passed the House in November included funding offsets such as charging wealthy seniors higher Medicare premiums and raiding an Obamacare disease prevention fund.
That bill did not go anywhere in the Senate. The Senate Finance Committee passed its own CHIP bill in October, but it did not include funding offsets and was never brought to the Senate floor.
States were forced to use funding leftover from the prior fiscal year as a stopgap. Congress also gave states $3 billion in short-term funding during a Dec. 22 continuing resolution to fund the government until Jan. 19.
Akler said states were worried that the program was being eliminated for good.
“There was a lot of publicity about how CHIP might end, and some states even sent out notices to families saying their coverage might end,” she said. “What we are concerned about is there may have been a chilling effect on enrollment, but we just don’t know.”
She added that states weren’t doing any outreach when they didn’t think they would have any funding.
“States now have certainty to start getting the word out that Medicaid and CHIP are open for business for children,” she said. “That is gonna take some work.”