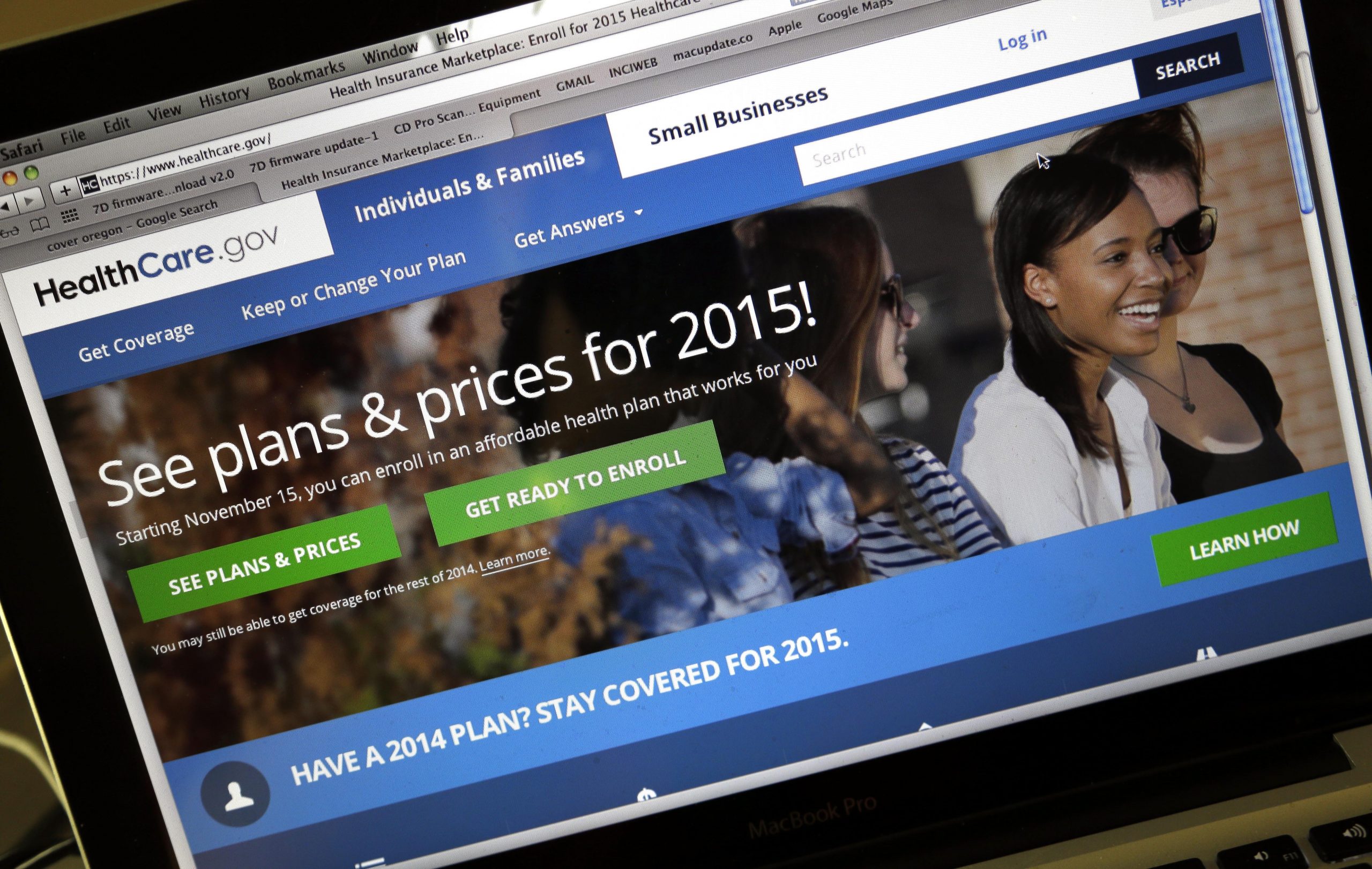
President Obama’s healthcare law aimed to make notoriously confusing health insurance policies clearer for consumers.
Recommended Stories
But despite some requirements for insurers to explain medical benefits in plain English, health advocates are still frustrated by a lack of transparency.
In a report released Thursday by the Kaiser Family Foundation, researchers found that some insurers aren’t fully complying with the law’s mandates to cover birth control but were unable to ascertain coverage policies from others.
“What did we learn? Getting this information is really difficult,” said Laurie Sobel, a senior policy analyst for Kaiser.
Insurers are mandated by Obamacare to give customers a form explaining how they cover health services. But the form is so opaque that it is having to be redesigned.
Kaiser reviewed how 20 plans cover different kinds of birth control. Not a single type of birth control coverage could be clearly explained by all the insurers providing it.
Half the plans wouldn’t clarify whether they charge co-pays or place other limits on coverage for intrauterine devices and half wouldn’t detail coverage policies for female sterilization. Officials with just nine of the plans agreed to sit down for interviews to talk about coverage policies. Researchers reviewed publicly available documents for the other 11.
If it’s difficult for full-time researchers to get the information, it’s obviously even harder for consumers to gain access to it. The National Women’s Law Center has set up a hotline for women to share their difficulty in accessing no-cost birth control through their insurer, as the health law requires. Gretchen Borchelt, the group’s vice president of health policy, said they get stories every day.
“These women are spending hours on the phones with insurance companies trying to figure out what their policy is,” Borchelt said. “They’re getting the run-around, they get conflicting information.”
The Obama administration said Thursday it is troubled by reports that insurers aren’t fully complying with the birth control requirements. The mandate is aimed at ensuring women don’t have to pay out of pocket for any type federally-approved birth control.
Katie Hill, a spokeswoman of the Department of Health and Human Services, said the agency plans to “release more guidance soon.”
But that won’t solve the challenges consumers face when they try to understand what their health insurance plan covers or doesn’t cover. That’s a remaining gap, said Edward Anselm, medical director of Health Republic Insurance of New Jersey, a nonprofit health plan.
“Even though we provide the information, people don’t have time to read a thick document and find out what part of it is for them,” Anselm said.
The form insurers must provide, known as the Summary of Benefits and Coverage, is supposed to help solve that. It’s the only standardized form that allows benefits to be compared side by side.
It is being redesigned, with heavy input by the National Association of Insurance Commissioners. It was supposed to be finished in September, but the federal government pushed back the deadline until at least Jan. 1, 2017.
Lynn Quincy, associate director of health reform policy for the Consumers Union, says one of the most consumer-friendly parts of the form is that it is required to provide two examples of how the plan would cover benefits for specific conditions, such as pregnancy or diabetes.
But she would like to see the form contain more than just the two coverage examples. And she would like the form to display a plan’s premiums more clearly and link directly to the list of drugs the plan covers.
“There are a whole bunch of rules about how they’re supposed to be filled out, but I think they could go a lot further,” Quincy said.